Home News & Views Dying Matters: Inspiring Others
Dying Matters: Inspiring Others
Kate Sanders, FoNS Practice Development Facilitator

A blog in support of Dying Matter Awareness Week 2018, written by Kate Sanders on behalf of the Teaching Care Homes teams.
During a recent Teaching Care Homes (TCH) programme workshop, one of the participants, Michelle, shared with us, that she had spent several months developing her own advance care plan. The desire to do this was stimulated by a trip to an experiential training session at a local undertakers, to find out what happens when someone has passed away. Here Michelle witnessed an embalming. She found the process detached, impersonal and distressing. This wasn’t because the undertakers were unprofessional; in fact, it was their very professionalism which upset her. The experience prompted Michelle to consider her own end of life. She has always feared being dead – not the experience of dying but of being dead. She started to think of how she could approach her own death in a way that gave her the assurance that she would be at peace. The events following her death needed to be planned in a way which gave her a choice which was shared with her family and acted upon. Since then Michelle has been compiling a book outlining her wishes and this is a work in progress and one which is part of family discussion. The research she has undertaken has opened her eyes completely to the fact that there are alternatives out there and we are largely ignorant of them.
This revelation sparked a significant amount of interest in the room and in the spirit of our ‘co-creation’ ways of working, we agreed to spend some time discussing this. Michelle talked more about the process that she had undertaken and all the different options for care at the end of life that she had learnt more about. She feels particularly strongly about the need to talk more about end of life care as she recognises that not everyone finds it easy to raise this subject with residents and their families. This view is supported by Macmillan (2017) who believe that many of us face barriers that stop us talking about dying. Michelle hopes that by creating and sharing her advance care plan with others, this will offer an opportunity for people to talk about choice at the end of life and also to raise awareness of all the possibilities there are for personalising care.
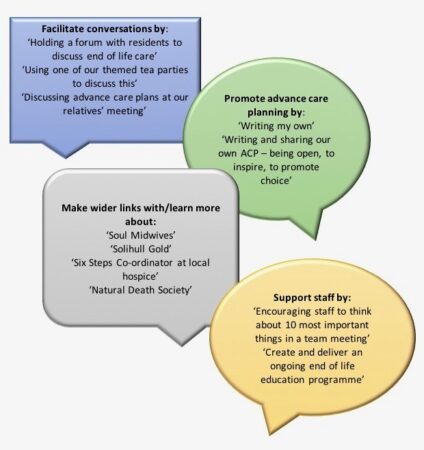
This discussion led to further conversations about what end of life care looked like in each of our homes; what had supported the development of good practice, but also in light of this conversation, what the opportunities for further improvement could be. Following this, we spent some time considering what actions we now wanted to take as individual care homes. As inspiring others is one of the priority areas that we want to explore and develop as part of our involvement in the TCH programme (see blog from 17th April 2018), we decided that we wanted to share our actions more widely, to encourage others to think about end of life care. The ideal time to do this seemed to be during Dying Matters Awareness Week 2018, so we hope that you will enjoy reading about our ideas below.
We have also come up with some resources that we have found useful or are going to make links with or find out more about. If you have ideas resources that would be helpful, please share through the comments box at the end of this blog. We look forward to hearing from you.
 Resources:
Resources:
Macmillan Cancer Support (2017) ‘No Regrets’: How talking more openly about death could help people die well This report explores issues such as death as a ‘taboo’ subject and the role of planning in improving care for people who are dying.
Marie Curie – Improving End of Life Care – Innovation and Resources This website provides a variety or reports relating to end of life care.
Namaste End of Life Care Programme for People with Dementia This website provides information about Namaste Care, but also access to a TedX Talk by its founder, Joyce Simard, and many free-to-access publications.
National End of Life Programme (2015) What’s Important to Me. A review of choice in end of life care This report identifies the issues that people approaching the end of life are currently facing and offers a blueprint for how greater choice in end of life care can be achieved.
The National Gold Standards Framework (GSF) Centre in End of Life Care: Library, Tools and Resources A library of resources including a template to facilitate a discussion about Advance Care Planning.
The Natural Death Centre This website shares knowledge with the intention of dispelling myths and empowering everyone who wants to have the best experience possible when it comes to making arrangements for a funeral.
Six Steps+ Programme The Six Steps + Programme is a series of workshops developed by the St Luke’s education team, designed to provide care homes and agencies with a toolkit to provide quality end of life care that meets CQC end of life essential standards.
Solihull Gold for Care Homes A closed Facebook group to create a community of empowered nurses who provide safe effective compassionate care, putting the residents at the centre.
Soul Midwives Soul Midwives draw on traditional skills, now largely forgotten, applying them to our modern world to lovingly ease the passage of the dying, and to ensure that their death is a dignified and peaceful experience. Their services are used within people’s own homes, in hospices and care homes. The website provides information about the practice of soul midwifery, details of training courses and lectures, and other helpful resources.
Comments are closed.

